These are handy point for reviewing before the exam . These points will help the medical student...
Medical Study Notes
Here are concise, exam-focused notes on Blood Physiology organized in clear bullet points 👇 🩸 Blood Physiology...
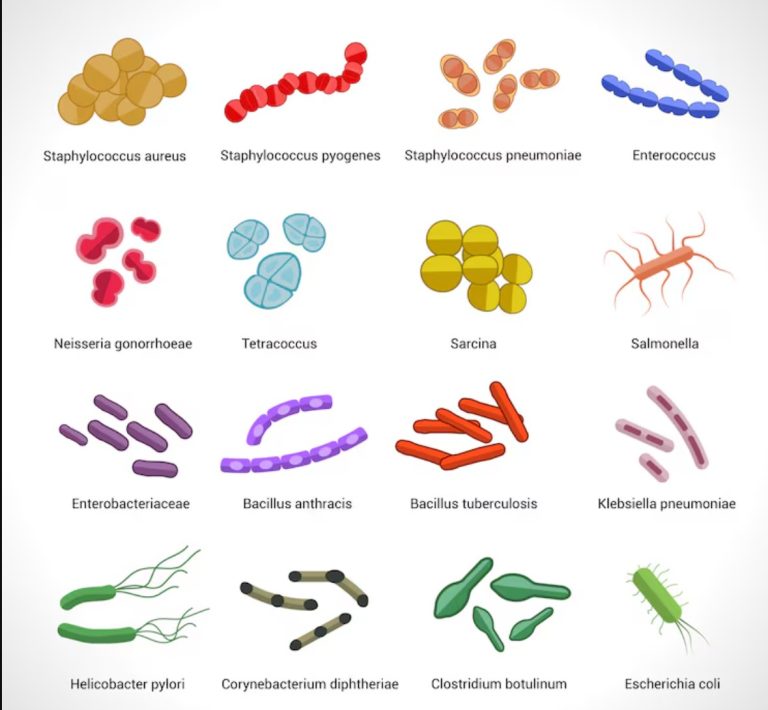
Here is a list and a table of the most common organisms associated with various clinical conditions, organized by...
Important ENT Notes for Exam Review are collections of major notes for medical students, especially MBBS...
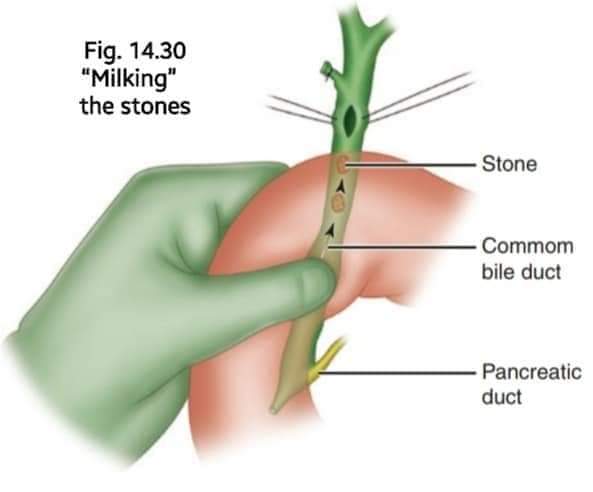
The trans-duodenal approach for CBD stones is a surgical technique used by the surgeon during the operation...